Global Point of Care
Changing the face of cardiac surgery
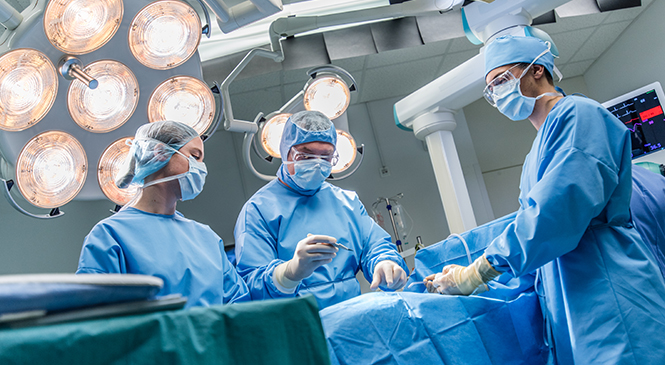

A country’s healthcare needs change over time, and as our population gets older, its healthcare needs become more complex.1
Nothing demonstrates this more than the increase seen in recent years in the number of cardiac surgeries. There are now more than one million cardiac surgeries annually across the world, and it is likely that this number will continue to rise.2
Cardiopulmonary Bypass (CPB) is a technique that temporarily takes over heart and lung function during surgery, maintaining the circulation and oxygenation of the patient’s blood.
Whilst patients are on Cardiopulmonary Bypass, they are most vulnerable and highly dependent on the skill of the clinical team and the technology that assists that team. During a typical cardiac surgery using Cardiopulmonary Bypass, patients will undergo a high number of tests, such as haemoglobin, haematocrit, blood gases and electrolytes. From induction of anesthesia until the immediate post-operative period, patients will typically have their blood drawn and analyzed every 20-30 minutes.2
“There are now more than one million cardiac surgeries
annually across the world”2
Utilizing ACT
ACT is traditionally measured in the operating room, as there is no laboratory equivalent test. However, the other blood tests required to monitor the patient safely during cardiac surgery are often analyzed outside the operating room, but within the confines of the surgical unit using point-of-care technology. This means the anesthetic assistant may be out of the operating room as much as 45 minutes, or even longer in more complex cases.
If a central hospital laboratory is used instead of point-of-care technology, history has shown that after the sample is drawn, the clinical team will not have access to a result for as much as 90 minutes.3 Waiting this long for a result means decisions are made based on historical data which may no longer reflect the true clinical picture. This could lead to delays in appropriate treatment.
The practice of with-patient testing involves using the blood analyzer at the patient’s bedside. This allows the blood sample, and more importantly, the anesthetic assistant, to remain in the operating room. The processing of blood samples takes place during the surgery, which means in times of crisis, a full complement of staff is available in the operating room. It also ensures a timely response to changes in the patient’s condition and reduces the likelihood of samples that leave the OR getting mixed up and reduces the likelihood that results are relayed to the wrong patient.
“A single device provides standardization, as well as simplification of connectivity issues.”
Devices that allow a broad menu of tests to be analyzed on a single platform can have a significant role in cardiac surgery operating rooms. A single device provides standardization, as well as simplification of connectivity issues the use of multiple devices creates, as well as providing a single footprint so as not to contribute to the already technologically overloaded operating room.
Conclusions
Cardiac surgery is becoming more complex and advances in technology must keep pace with these demands so that clinical teams are equipped to deliver the best possible standard of care. With-patient testing provides a simple solution to intraoperative blood testing that allows staff members to remain in the operating room and deliver care in a safer and more timely manner.
References
- Afilalo J et al. Addition of fraility and disability to cardiac surgery risk scores identifies elderly patients at high risk of mortality or major morbidity. Circ Cardiovac Qual Outcomes 2012, 5(2):222-228
- Falter F. Benefits of handheld diagnostics in the CVOR. Hospital Healthcare Europe, 2015
- National Institute for Health and Care Excellence. Detecting, managing and monitoring haemostasis: viscoelastometric point of care testing. August 2014. www.nice.org.uk/guidance/dg13


