Global Point of Care
SEPSIS, BY THE NUMBERS:
what are average costs and where can you save?
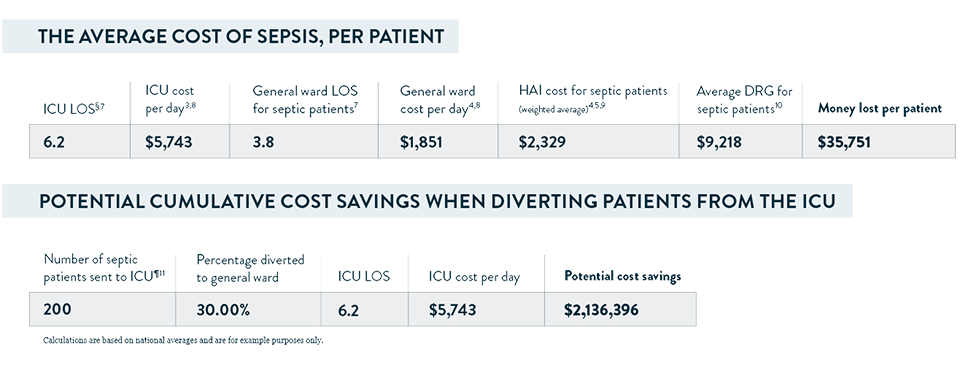
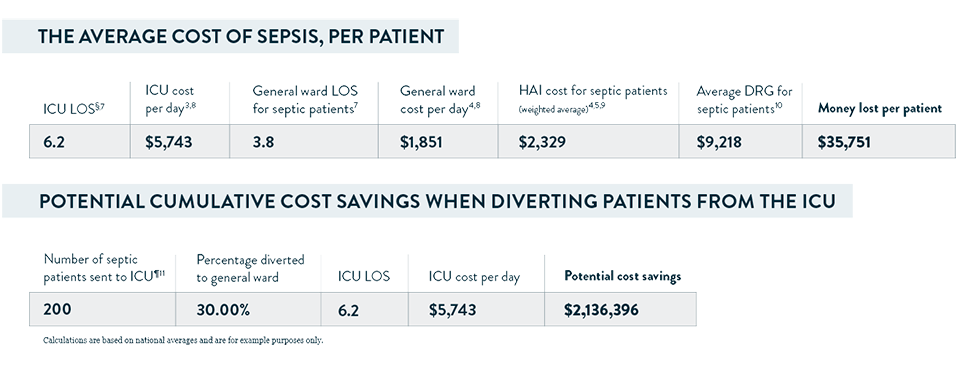
The table below shows average sepsis costs. See how much your facility can save by downloading the free calculator pdf.
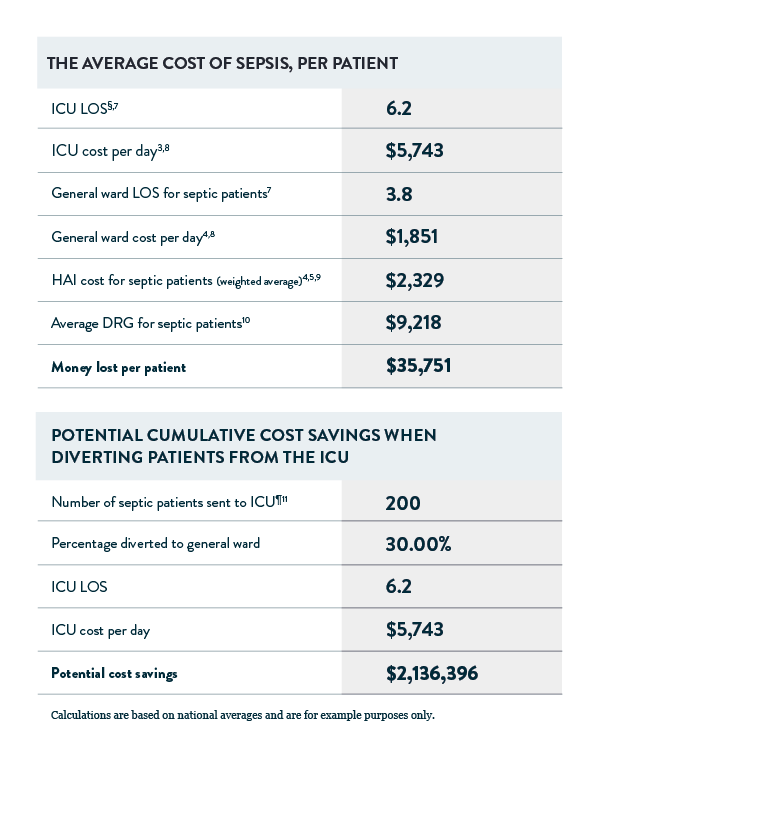

References
*Estimated annual healthcare cost for the approximately 125,000 suspected sepsis patients unnecessarily admitted to the ICU
†$44,969 weighted average cost for each septic patient, minus $9,218 weighted average DRG per septic patient
‡Compared with lab testing
§Based on the average LOS for severe sepsis, the most common sepsis DRG (comprising 70% of all sepsis cases)
¶Based on 500 bed hospital; 33.91% of patients diagnosed with sepsis in ED are admitted to ICU
- Klein Klouwenberg PMC, Cremer OL, van Vught LA, et al. Likelihood of infection in patients with presumed sepsis at the time of intensive care unit admission: a cohort study. Crit Care 19, 319 (2015). https://doi.org/10.1186/s13054-015-1035-1
- Kuye I, Rhee C. Spotlight: Overdiagnosis and delay: Challeges in sepsis diagnosis. 2018. https://psnet.ahrq.gov/web-mm/spotlightoverdiagnosis-and-delay-challenges-sepsis-diagnosis. Accessed 12/3/21.
- Paoli CJ, Reynolds MA, Sinha M, Gitlin M, Crouser E. Epidemiology and Costs of Sepsis in the United States-An Analysis Based on Timing of Diagnosis and Severity Level. Crit Care Med. 2018;46(12):1889-1897. doi:10.1097/CCM.0000000000003342
- Agency for Healthcare Research and Quality. Healthcare Cost and Utilization Project. 2018 National Medicare-Severity Diagnosis Related Groups (MS-DRG), Principal: #870 Septicemia or severe sepsis w mv 96+ hours, #871 Septicemia or severe sepsis w/o mv 96+ hours w mcc, #872 Septicemia or severe sepsis w/o mv 96+ hours w/o mcc. https://tinyurl.com/2p8e5bp9 Accessed 12/21/21.
- Halpern NA, Pastores SM. Critical Care Medicine Beds, Use, Occupancy, and Costs in the United States: A Methodological Review. Crit Care Med. 2015;43(11):2452-2459. doi:10.1097/CCM.0000000000001227
- Economic conversion by Akash Bijlani, MPH, Strategy Access Solutions, based on data available at https://beta.bls.gov/dataViewer/view/timeseries CUSR0000SAM2;jsessionid=2251CA2D2963638EE832EB247E342883.
- Halpern NA, Pastores SM. Critical care medicine in the United States 2000-2005: an analysis of bed numbers, occupancy rates, payer mix, and costs. Crit Care Med. 2010 Jan;38(1):65-71. doi: 10.1097/CCM.0b013e3181b090d0.
- Hassan M, Tuckman HP, Patrick RH, Kountz DS, Kohn JL. (2010). Hospital length of stay and probability of acquiring infection. Int J of Pharm and Healthcare Marketing, 4(4), 324-338. https://doi.org/10.1108/17506121011095182
- Van Vught LA, Klein Klouwenberg PM, Spitoni C, et al. MARS Consortium. Incidence, Risk Factors, and Attributable Mortality of Secondary Infections in the Intensive Care Unit After Admission for Sepsis. JAMA. 2016 Apr 12;315(14):1469-79. doi: 10.1001/jama.2016.2691.
- Wang HE, Jones AR, Donnelly JP. (2017). Revised national estimates of emergency department visits for sepsis in the United States. Crit Care Med, 45(9),1443-1449.
- Wang HE, Jones AR, Donnelly JP. Revised National Estimates of Emergency Department Visits for Sepsis in the United States. Crit Care Med. 2017 Sep;45(9):1443-1449. doi: 10.1097/CCM.0000000000002538.







